Diarrhea (or diarrhoea) is a common traveller's illness. To some extent, it's unavoidable: no matter how fanatical you are about food preparation, it's still liberally sprinkled with millions of airborne bacteria. At home, due to this constant exposure to the local germs, odds are very high that you're already immune to them. But in other parts of the world, where the bacteriological fauna are new to you, you're far more likely to run into problems. Also, in warmer climates bacteria both reproduce more quickly and survive longer outside the body. Thus the scourges of Delhi Belly, the Pharaoh's Curse, Montezuma's Revenge, and their many friends.
As with respiratory problems in colder climates, intestinal problems in hot climates are fairly common and in most cases are distinctly annoying but not really dangerous. Take it easy while feeling miserable for a few days, drink lots of fluids, and usually you will soon be well.
There are vaccines against many of these, including cholera, typhoid and rotavirus. Consult a doctor several weeks before your planned travel, giving time to have any vaccines you need.
Understand
editUsually the traveller's affliction is gastroenteritis, an inflammation of the stomach tissue (gastritis) or the small bowel (enteritis) or both, which causes abdominal pain and frequent watery stools. There may also be vomiting and fever. The commonest cause is viruses, but bacteria or protozoa can cause nearly identical symptoms. These are transmitted via fecal-oral contamination – contaminated water, shellfish from such water, contaminated food, dirty toilets, etc. – and the main defense is good hygiene.
A typical intestinal infection is quite unlikely to kill, though a patient may feel like it is going to, or even wish it would. However, as for apparent colds that might turn out to be pneumonia, some more serious diseases have intestinal upsets as their first symptoms. It is very important to monitor the symptoms and see a doctor if the condition persists or if unusual symptoms appear. Things to watch for are:
- the acute symptoms persist for more than two days, or
- there is blood or pus in your feces, or
- the feces are black, which is caused by blood, or
- fever goes over 39 °C (102 °F), or
- you are getting chills as well as fever, or
- the pain evolves beyond a nauseous kind of sick, or
- other weird symptoms show up, e.g. skin marks
If such symptoms appear, then you may have something worse and should see a doctor. Do not try to just fight it off. According to WHO, diseases involving diarrhea kill more than 1.5 million people a year, so if you have signs of more serious illness, take them seriously. Of course in many cases the doctor will tell you it is not in fact serious, but do check.
Prevent
edit
There's an old adage for eating in the Third World:
- Boil it, cook it, peel it, or forget it.
This seems simple, but in practice it's a tough road to follow, the problem being not so much the risk of accident as the risk of temptation. For example, the following items are highly likely to cause problems:
- tap water
- ice
- milk
- fresh fruits and vegetables, especially leafy vegetables
- raw eggs (as in mayonnaise)
- meat that is not well done
- raw fish and seafood
Test: It's another sweltering hot day in Delhi and that curry you just ate is still scorching your throat, so how about a nice strawberry shake to cool you down? If you said "Sure!", you may just have passed an intestinal death sentence on yourself: that shake contains as many as four of these high-risk items. The ice that makes it cold has either been made from tap water or, worse yet, comes from the factory in huge blocks that are often literally dragged down the street. Milk spoils very quickly in the tropics. And those yummy leafy veggies and unpeeled fruits have been washed in that same parasite-laden tap water... if at all.
Having read this, your instinctive reaction will be to panic and to head for the nearest expensive, air-conditioned tourist restaurant. Bad move. They're still using the same ingredients, stored with the same levels of hygiene or lack thereof, but because it's a tourist restaurant their business model relies on catching a couple of tourists a day, instead of feeding a crowd of locals. This, in turn, means that those same ingredients have, more often than not, been sitting around a long time waiting for you.
What to do then? It's a numbers game, but here are a few guidelines to improve your odds of escaping unscathed:
- Choose local food. That's what they know how to handle. Don't go to that fancy tourist restaurant to have that steak or Russian salad you can eat at home and which they have absolutely no idea how to handle properly.
- Choose a popular restaurant. Many people (especially locals!) means that the food isn't left sitting around, and more likely than not, it also means the chow is good and the price is right.
- Be careful with street stalls. Often they lack running water, hygiene may be poor and the food may be exposed to street dirt.
- Choose cooked dishes that are made on demand. Things like fried rice and fried noodles are popular in the tropics for a reason. Buffet-style meals, on the other hand, may appear cheap but are very risky.
- Dishes that are kept boiling hot – in practice this means hot drinks and soup – are also a pretty good option.
- Spicy food such as fiery curries and the like is usually OK since they're cooked, and the capsaicin in it acts as a natural disinfectant. On the flip side, excessive spices alone may be enough to upset your stomach's balance, so it's best to avoid these at least for the first few days if you're not used to them. Some shady restaurants use excessive spice to mask expired meats, if this is the case there is a good chance dishes where spice is not normally used will be highly spiced. Of course some legitimate restaurants will add spice in unorthodox ways too.
- Avoid meat, fish, and especially shellfish; meat is often purchased from unsanitary open-air markets, where the chances of it harboring germs or disease are dramatically increased. Eating ground meat (meatballs etc) or anything not well-done is especially risky, not only due to food poisoning but because of the risk of things like trichinosis. Additionally, things like barbecues and roast chicken have to be prepared in advance, and who knows how long they have been sitting there?
- Drink only beverages from untampered bottles and cans, and check the seals first! Don't let waiters pour stuff in the kitchen. Reputable restaurants will open their drinks in front of you for this very reason.
- Heat fresh milk thoroughly before drinking it, or use condensed or powdered milk instead. If you are mixing up powder (formulae milk) boil or sterilise the water used first. Milk should be slowly heated to 72 °C (162 °F) and held there for at least 15 seconds; don't heat it too fast as it will cause the milk to curdle.
The good news is that in a couple of days you'll start to acclimatize to the local bacteria and your odds of getting sick will start to decrease. The bad news is that it only takes one fly in the wrong place at the wrong time to foil all your precautions, and that if you stick around for a while, a run-in with food poisoning is, alas, more or less inevitable.
Dukoral is an oral cholera vaccine that also gives some resistance to diarrhea caused by enterotoxigenic E. coli (ETEC). It is only partly effective, so still take all the other precautions as well. It is available over the counter in a few countries and states and by prescription in others.
Treat
editSo one day your luck runs out, and you find yourself feeling distinctly queasy. Runny bowels or simple diarrhea don't really qualify for food poisoning, but if you...
- feel sick and dizzy
- get a fever
- start to feel like you need to throw up
...then, well, you're reading the right article. The first thing to do is to get the acute phase over with: head for the toilet, kneel in front of the bowl and let go. You won't start to feel better until you start throwing up, and you won't get this over with until your stomach is empty, so just do it. Do not attempt to eat anything, and do not drink anything other than water yet. When there's nothing left, wash your mouth, brush your teeth and go to bed. You'll feel more alive in the morning.
Drink
editAny form of diarrhea can cause dehydration; see the linked article for more detail. You're losing fluids constantly from any number of orifices, and your symptoms will become worse if you start to dry out. Headache or dark-coloured urine are common signs of dehydration.
For mild cases of dehydration, plain water, oral rehydration mixture (available from pharmacies), weak tea (sweetened), flat soda, and some diluted fruit juices are all good (but avoid vitamin C). Drinking a glass or two an hour till everything stops running out the other end should stop you becoming too dehydrated. Aim for drinks at room temperature. Do not drink caffeinated drinks or alcohol. Carbonated drinks should be allowed to go flat before drinking.
If you are vomiting intermittently, you should drink in regular sips rather than one big glass or more of water. Start sipping about half an hour after each vomiting episode.
Eat
editFor the next few days, you will find that your appetite has all but disappeared. Don't force yourself to eat. If you feel like eating something, stick to bland, stomach-friendly foods like rice, porridge, crackers, and bread. But be aware that food for you is also food for any bug that has made you sick, so take it slowly and stop if things get worse. Eat to match your appetite: Don't chuck down large quantities of food to make up for the last few days, instead eat small portions spread out over the day.
Avoid oily foods and most dairy products. Yoghurt and similar products, however, are OK since the lactobacteria have broken down the hard-to-digest parts.
Some people find that — as a preventative or in treating mild cases — yoghurt, buttermilk and similar products help. They are bacterial cultures; the hope is that their benign bacteria will overwhelm the nasty ones (and replace some that you lost during the sickness). Choose a "natural" product: most flavoured yoghurt has been heated, killing the culture. This is a fairly well established idea in travellers' folklore but attempts to confirm it scientifically have not given clear results. Do not try this if you are acutely ill; you will just heave up the yoghurt and feel even worse.
Though much oily food can cause diarrhea, it actually might be best to eat from international food chains (McDonald's, etc). These restaurants tend to follow strict sanitary rules. However, if the restaurant looks questionable and unclean, don't eat there.
Medicate
editMost experienced travellers in high-risk areas carry an antidiarrheal drug (often loperamide, sold as Imodium and other names) as a safety precaution. It can be quite difficult to get to a pharmacy if you are ill, so it is sensible to be prepared. These can provide considerable relief from the symptoms of an upset stomach, but they do nothing to cure the disease.
It is usually wisest not to take an antidiarrheal just to get some relief. You are likely to recover more quickly if you just endure the discomfort, drink your fluids, and let your body get on with the business of expelling the nasty stuff.
Where these drugs become essential is when you have something to do that will mean you have no easy access to a toilet, e.g. your visa is expiring so you must go renew it or you have a flight booked. Even then, it is definitely not a good idea to use these drugs for more than a day or two at a time; with no output your innards can become severely clogged, which will be quite uncomfortable and may even be dangerous in extreme cases.
About the only other treatments you might try without medical advice are Bismuth subsalicylate (Pepto-Bismol) to soothe the stomach, and ginger which is a natural remedy against vomiting. Either may provide some relief without blocking anything up if diarrhea is not too serious. Don't take aspirin (acetylsalicylic acid) to calm things down — aspirin requires a healthy stomach.
Other drugs may also be used, but usually should not be without a doctor's advice:
- An antiemetic reduces or eliminates vomiting.
- An antispasmodic reduces painful spasms in the digestive tract.
- Metoclopramide (MCP) or domperidone (both sold under various names) will stimulate bowel movements, reducing stomach pain and nausea while facilitating natural expulsion of the bad stuff. In most countries you will need a prescription for MCP, in some also for domperidone.
- Antibiotics may be prescribed in severe cases. However, a common side effect of antibiotics is diarrhea – take only as prescribed by your doctor.
On no account take antibiotics without consulting a doctor first! One problem is that antibiotics are completely useless against viral infections. Another is that they kill off microbes that are needed as part of the digestive process. Most important, overuse or improper use of antibiotics helps create resistant microbes.
Treat others
editIf your travelling companions are down for the count, the best thing you can do for them is supply them with water and rehydration solution, and, alas, possibly clean up after them. Wash your hands with very warm water and soap after cleaning, touching the sufferer, handling their clothes or bedding, and of course before eating.
Some groups of people are very vulnerable to dehydration after developing diarrhea. In particular, because of their small bodies, toddlers and babies dehydrate extremely quickly; elderly people also dehydrate more quickly than young adults, and any illness is serious in someone immunocompromised (eg, by AIDS or chemotherapy). A baby with diarrhea should be taken to the doctor immediately if it is under 3 months old, and also if it is older and is either vomiting, has a fever or has stopped wetting its nappy regularly, as this means it is dehydrated.
Remember to bring sufficient baby wipes, much stronger than toilet paper.
Don't share
editOnce sick with vomiting and/or diarrhea do not, if at all possible, prepare or handle food that other people intend to eat as you may infect them with your illness. Continue not to handle others' food for at least 2 days after the symptoms are gone. Sufferers should be extra vigilant about washing their hands thoroughly with warm water and soap before meals and after using (or cleaning) the toilet to make sure the germs do not spread.
|
Do not mix cleaning products.
Most cleaning products contain strong chemicals and require routine precautions such as keeping them out of reach of children, wearing gloves when using them, and rinsing well afterward. See their labels for details. Using two cleaning products at the same time is a terrible idea because there may be a chemical reaction between them. This reduces the effect of both, some of the reactions may be violent, even explosive, and some produce even more dangerous chemicals. In the worst case — using bleach with some toilet cleaners — the reaction releases chlorine gas which can be fatal. If you think the job needs more than one cleaner, apply one, rinse thoroughly, then apply the other. |
Avoid using the same toilet with an infected person if you can. Reserve and quarantine one toilet for the use of the infected person (it still has to be kept clean, though) and use another one for yourself (or make sure the others use it if you are the one who is sick). If this is not possible, you (or someone else) have to use the same toilet with someone sick, disinfecting the toilet with household bleach after each and any use (defecating, urinating, throwing up, you name what else) by the infected person is a wise precaution. Although not very environmentally friendly, household bleach is generally the cheapest and most common option available (it has different names in different countries (for example eau de Javel in French-speaking countries, after the name of the town which it was first produced), if you don’t know the local name, check the label, it will state that it contains “sodium hypochlorite” (substitute “natrium” for “sodium” in some of the Germanic-, and Slavic-speaking countries), sometimes with the percentage: up to 5%). Pour the bleach on every part of the toilet bowl that was possibly in contact with the bodily wastes after all the solid dirt is removed (solid material hinders disinfecting properties of bleach). Don’t flush bleach down immediately, let it sit for at least 5-10 minutes so it has enough time to kill the nasty bugs.
Some food-related illnesses can spread rapidly through groups of people particularly where the group is regularly gathering for meals. If you are travelling in a group of people (particularly in a closed environment like a cruise ship) or attending a conference or similar gathering it is good to inform the organisers or medical staff if any of your illness so that they are alert to a possible problem for everyone else.
Complications
edit- See also: Infectious diseases
Sometimes a bout of diarrhea is the first symptom of something worse. If you have reason to suspect any of these, see a doctor, as the following conditions require medical care.
Cholera
editCholera is an extreme form of diarrhea, identifiable by torrents of liquid stool with white flecks of mucus ("rice water stools"). The skin and lips may turn dark and the eyes may sink due to dehydration. The disease is caused by the Vibrio cholerae bacterium and is generally transmitted by unsafe drinking water or food. Historically, it was one of the major killers; some cholera epidemics wiped out hundreds of thousands.
What kills is dehydration; untreated cholera kills more than half of its victims, often within 24 hours. Re-hydration is the main treatment; that alone reduces the risk of death to under 5%. Often intravenous fluids are required as well as fluids by mouth, since a cholera patient can lose over a liter of fluid an hour via diarrhea and it is hard to drink enough to replace that, and to keep it down if you do. Antibiotics may also be used.
Today the disease is rare in most places, but still present in the Indian subcontinent, Southeast Asia and parts of Africa; it still affects 3–5 million people a year and kills tens of thousands. Almost anyone planning travel to areas with cholera risk should get a vaccination; consult a doctor for details. Vaccines have been available for some decades, nowadays oral as well as injected. None of them gives full protection or is effective for more than 2-3 years. Three oral vaccines – Dukoral, ShanChol, and Euvichol – have WHO approval, but in the US only Vaxchora is FDA-approved as of mid-2020. Dukoral also provides partial protection against some other stomach infections.
Dysentery
editDysentery is an inflammation of the intestines resulting in diarrhea with blood or pus in the feces, often accompanied by fever or painful stomach cramps. The most common visible sign of intestinal bleeding is that the feces are black. Dysentery occurs more commonly in the tropics and is closely linked to poor hygiene; it remains a devastating illness in much of the Third World, but can be easily treated with modern medicine. There are two major causes:
- Bacillary dysentery (or shigellosis), caused by Shigella bacteria. Transmitted through fecal-oral contact, with time from exposure to symptoms being 12-50 hours.
- Amoebic dysentery (or amoebiasis), caused by the Entamoeba histolytica amoeba. Transmitted through contaminated water, can remain dormant for a long time and only appears after a period of weeks or months.
Dysentery can be confirmed by a stool test, but differentiating the bacillary and amoebic types takes at least 48 hours, so medication for both is often started simultaneously. The condition can usually be cured with five days of treatment with antibiotics (for bacillary) or metronidazole (for amoebic), and hospitalization is usually only necessary if fluid loss is extreme. The stool in dysentery can be highly contagious, so frequent handwashing for caregivers is essential.
Typhoid fever
edit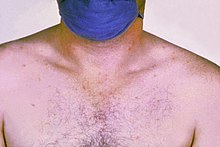
Characterized by slow buildup, up to a week, to high fever (40°C) with heavy sweating and, in later stages, delirium. Diarrhea is green and bloodless; however, some people have constipation instead. Caused by the Salmonella bacterium, identified by blood or stool test, and usually easily cured with antibiotics. Untreated cases have 10-30% fatality rates and even the survivors may be thoroughly miserable for up to a month.
Vaccination is recommended for travellers to certain countries, including most of the "Third World". Both an injected and an oral vaccine are available; neither gives 100% protection.
Giardiasis
editAlso known as beaver fever, this can be identified by explosive diarrhea, foul-smelling flatulence and vomiting, often starting 1-2 weeks after infection and recurring in cycles. The cause is the Giardia lamblia protozoan, which is transmitted by the fecal-oral route, and often strikes people consuming untreated water in the wilderness and also in countries with poor hygiene. It can also be acquired from the tap water systems of some places, like St. Petersburg in Russia. Two-thirds of the people affected are silent carriers, and the condition often resolves with time. However, once identified, giardiasis can be cured with a single dose of tinidazole. Metronidazole is a common alternative in poorer countries, and is often available from pharmacies.
